About
Approximately 1 in 5 Canadians experience a mental health problem in any given year and, by age 40, approximately 50% of individuals will have experienced a mental illness. Most Canadians rely on their primary care providers to address their mental health needs. While this may be effective for many patients, there is a subset of individuals who present with a severity and complexity that requires specialist care. Unfortunately, a shortage in the number of psychiatrists – as well as an imbalance in their geographical distribution, particularly in rural and northern Canada– can result in wait times of months to years. In the meantime, primary care teams must manage these cases in settings not designed for specialized psychiatric care, creating a mismatch that can lead to provider frustration and potentially sub-optimal patient outcomes.
Emerging evidence suggests that educational initiatives and innovative ways of delivering psychiatric care may help address these structural obstacles. To this end, we designed The Alberta Network for Community Health Outreach and Rural Mental Health (ANCHOR-MH), a novel educational program with the goals of enhancing Family Medicine (FM) physicians’ confidence and skill at treating psychiatric illnesses, improving collaboration between FM physicians and psychiatrists, and establishing an enduring community of practice. This work and its early implementation are described in a recent Folio article.
Program Model
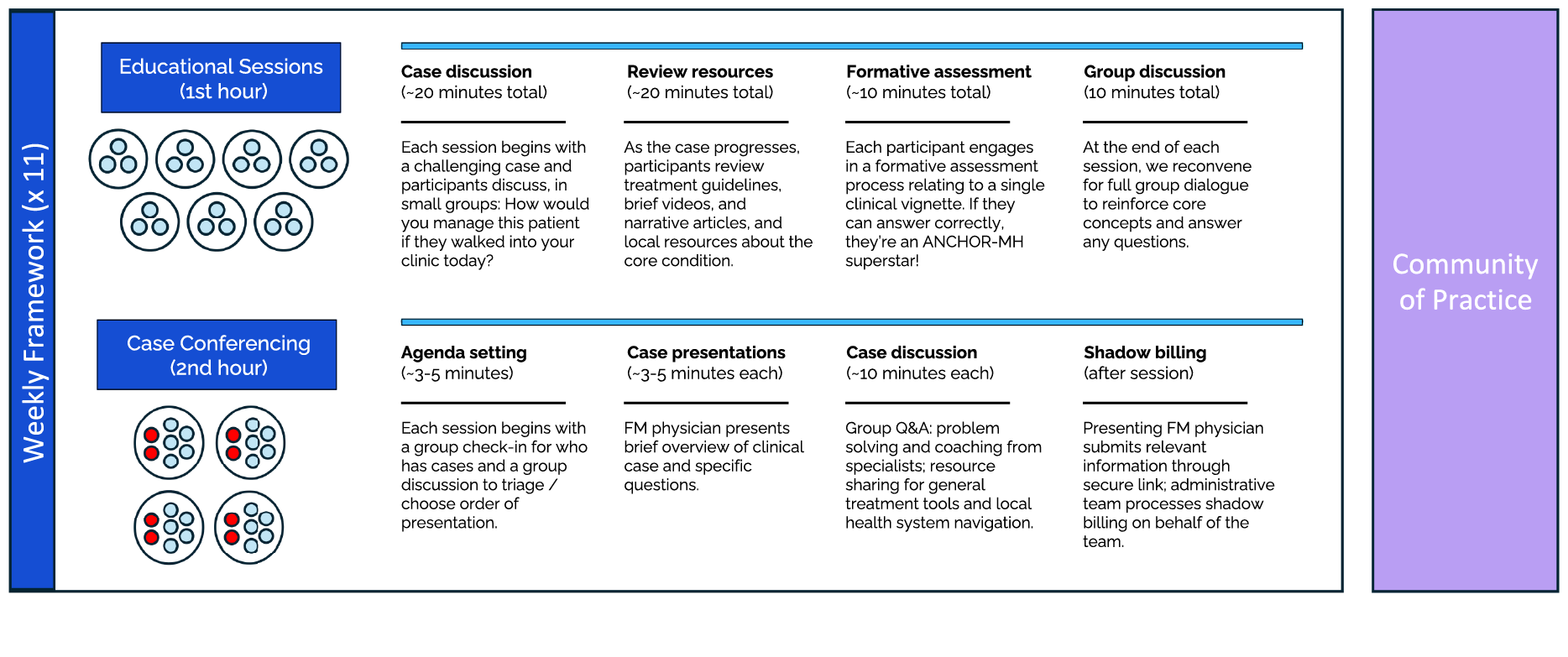
Each cohort operates in a tri-partite model that balances structured learning with real-world clinical application (see below). For each of twelve weeks, participating family physicians engage in focused educational sessions to deepen their expertise and leadership in mental health care. In parallel, they participate in collaborative case work, with groups of five family physicians consulting with two psychiatrists regarding current patients they treat for mental health concerns. This structure offers personalized instruction, supports complex decision-making, and extends psychiatric reach across a wider patient population.
The third component to the program is an asynchronous platform designed to facilitate a community of practice: participants can log in to find high-yield resources and clinical tools and to ask questions to peers and consultants. This structure also allows for ongoing case conferencing and coaching beyond the initial 3-month experience.
Who Can Apply
Clinicians who regularly care for patients with mental health concerns in primary care and are looking to strengthen their approach to complex cases are encouraged to apply. Participants collaborate with psychiatrists around real clinical work with the goal of improving patient care.
How to Apply
Clinicians who wish to submit a new application, carry forward a previous application, or be added to the wait list are asked to complete the application form below.
A full application requires a current CV and a brief letter of interest. Applications submitted without these materials will not be reviewed.
Applicants who have previously submitted a full application do not need to resubmit their materials, as files will be carried forward.
Clinicians who do not wish to submit a full application at this time may indicate their interest in being placed on the wait list within the application form. Supporting documents are not required for wait list consideration.
Applications are accepted on a rolling basis.
Meet the Team

David A. Ross
MD, PhD
Dr. David A. Ross is Professor and Chair of the Department of Psychiatry in the Faculty of Medicine & Dentistry at the University of Alberta. The primary focus of his academic work is on designing, implementing, and disseminating innovative educational resources. He is a Co-Founder and Executive Director of the National Neuroscience Curriculum Initiative, the goal of which is to help integrate cutting-edge neuroscience into psychiatry. Through this work, he has helped create a set of shared curriculum resources that are now in use at more than 200 programs around the world.
Dr. Ross is the Founding Director of the TIME4MH Initiative and helps lead the ANCHOR-MH and OASIS pillars, which aim to: enhance access to care; improve mental health outcomes, especially with historically underserved communities; and reduce stigma towards psychiatric illness.

Jeremy Weleff
DO
Dr. Jeremy Weleff, DO is a clinician-researcher and educator in psychiatry at the University of Alberta, with an adjunct appointment at Yale School of Medicine. His work focuses on addiction and substance abuse disorders, psychiatric epidemiology, and social determinants of health. He also collaborates with the Neuroscience and Mental Health Institute on community-engaged research aimed at supporting vulnerable populations.
Dr. Weleff is a key researcher in OASIS (Overcoming and Addressing Stigma In Substance Use Disorders), an ongoing study within the TIME4MH Initiative, that evaluates a community-facing educational intervention designed for clinicians and individuals with lived experience of opioid use, to reduce stigma and barriers to care, and improve treatment engagement and outcomes.
Prior to joining the University of Alberta, Dr. Weleff completed advanced training in public psychiatry and addiction psychiatry fellowships at Yale-affiliated programs, where he developed expertise in complex clinical care and innovative therapeutic approaches.
Dr. Weleff maintains active involvement in scholarly networks and services as a peer reviewer and research collaborator internationally, reflecting his ongoing commitment to advancing psychiatric science and improving mental health outcomes worldwide.

Khrystyna Lukyanets
Program Assistant
Khrystyna is the Program Assistant for ANCHOR-MH, supporting the planning and delivery of the initiative, including session coordination, participant onboarding, communications, and documentation.
Prior to joining the University of Alberta, she worked in not-for-profit programming, coordinating large-scale events and educational initiatives, and collaborating with community organizations and public sector partners on implementation and outreach.
She holds a Bachelor of Arts in English and Education, as well as a diploma in Chemical Engineering Technology.
Publications
Resources for Primary Care
We are developing practical tools to support clinicians navigating mental health services across Alberta:
Alberta Mental Health Clinician Wiki
A curated directory of referral resources and services to help clinicians quickly identify appropriate supports for their patients.
Contact
For more information, please contact:
